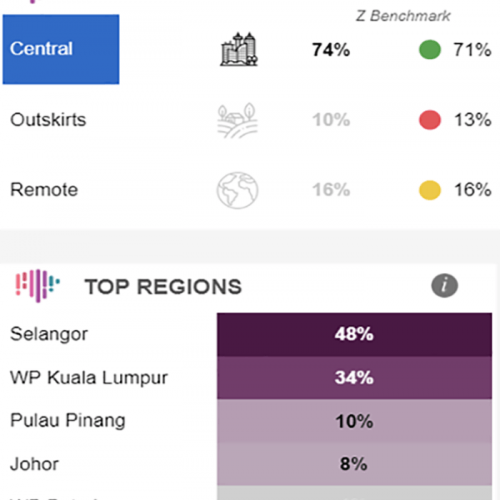
Box 藉由清晰呈現安全資料,有效打擊網路威脅
為了進一步強化內容與工作流程保護,Box 使用 Tableau Cloud 中的 Tableau Pulse 來提供見解、最佳化安全機制,以抵禦因 AI 濫用所衍生的新型威脅。

Customer Story
富國銀行處理 7,000 多萬客戶的資料,藉以重新設計客戶銀行入口網站
icon--resources">